Human Papillomavirus Vaccination: Narrative Review of Studies on How Providers' Vaccine Communication Affects Attitudes and Uptake
Adult and Child Consortium for Outcomes Research and Dissemination Science, and University of Colorado Denver
Much research has focused on understanding the reasons underlying low adolescent human papillomavirus (HPV) vaccination rates in the United States (US). In that light, this review examines the influence that provider communication techniques have on parental attitudes regarding HPV vaccine, as well as how those techniques affect vaccination uptake. In it, Drs. Dempsey and O'Leary:
- explore the limited literature that has directly measured the influence of provider communication techniques on parental attitudes;
- review the literature on the use of so-called "presumptive" recommendations, and how these types of recommendations are associated with increased HPV vaccine uptake;
- present new information regarding the use of motivational interviewing (MI) as a provider communication technique to improve vaccination uptake, particularly among vaccine-hesitant parents; and
- suggest "best practices".
As Drs. Dempsey and O'Leary outline, numerous studies have shown that a provider recommendation is one of the strongest predictors of adolescent HPV vaccine uptake. It is not enough to simply "make a recommendation"; the specific language the provider uses and the tone he or she uses to communicate their recommendation can have major effects on the likelihood that a vaccine is received. Studies have shown providers often fall short in fulfilling what Gilkey and collagues have advanced as 4 essential components of a "high-quality" HPV vaccine recommendation: (i) timeliness: routinely recommending the vaccine starting when the patient is 11 to 12 years old, (ii) consistency: recommending the vaccine for all eligible adolescents instead of preferentially vaccinating those perceived at high risk for infection, (iii) urgency: recommending that the vaccine is given the same day it is discussed, and (iv) strength: using unambiguous language that clearly conveys the importance of the vaccine.
They go on to look at 2 studies that directly examined how providers' communication strategies relate to parents' specific HPV vaccination attitudes. One suggests that the strength of a provider recommendation strongly influences parents' perceptions regarding the safety of HPV vaccine; the other indicates that brief recommendations might be best for parents without significant concerns.
Studies on the effect of providers' recommendations on vaccine uptake are reviewed that focus on:
- Presumptive recommendations: Data suggest that for many parents of adolescents, brief, direct language that normalises HPV vaccination might be an effective provider communication method.
- Making the recommendation "strong": Studies show that a strong provider recommendation, particularly one that is presented in a brief, normative format, is an effective method. However, future work might be needed to understand the specific language or other elements of a providers' HPV vaccine communication that create the perception among parents that the recommendation was a strong one.
- Using MI when parents are reluctant to vaccinate: Strong, brief, presumptive communication techniques for promoting HPV vaccination might not work for parents with significant vaccine hesitancy. MI, which describes a conversational style in which the provider leverages a patients/parents' intrinsic motivations for complying with a recommended health behaviour, has been shown to have promise in increasing vaccination. Future research will be needed to explore more fully the efficacy of this technique.
Along the lines of future research, looking at data compiled in the fields of psychology and decision-making may provide insights upon which researchers interested in promoting HPV vaccination can draw. These areas of research suggest that creative communication strategies such as focusing on leveraging parents' values (which are typically stable over time) rather than attitudes (which can change depending on the situation) and on using self-affirmation to improve vaccine-hesitant parents' willingness to hear pro-vaccine messages might be useful strategies. However, these communication approaches have not yet been applied HPV vaccination. Future research in this vein should engage multidisciplinary teams with expertise across diverse fields to apply the learning that already exists in the social sciences to the problem of vaccine hesitancy and refusal.
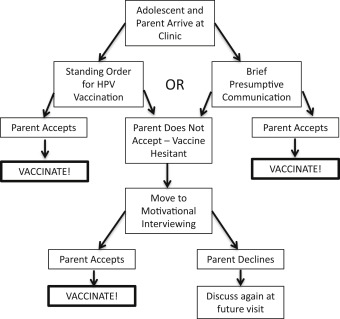
In conclusion, Drs. Dempsey and O'Leary suggest that promising, evidence-based communication techniques include using brief, strong, unambiguous language to introduce the HPV vaccine, followed by more nuanced communication techniques, such as MI, when encountering resistance.
Academic Pediatrics, March 2018, Volume 18, Issue 2, Supplement, Pages S23–S27. DOI: https://doi.org/10.1016/j.acap.2017.09.001.
- Log in to post comments












































