Addressing Barriers to Vaccine Acceptance: An Overview
Dalhousie University, Canadian Centre for Vaccinology, IWK Health Centre (MacDonald); WHO Regional Office for Europe (Butler); Institut National de Santé Publique du Québec (Dubé)
Of the 194 countries who completed the World Health Organization (WHO) and United Nations Children's Fund (UNICEF) Joint Reporting Form (JRF) in 2014, 74%% reported that vaccine hesitancy was an issue in their country. Though the problem seems to be widespread, there is no simple strategy that can address all the barriers to vaccine acceptance. Thus, overcoming hesitancy requires detection, diagnosis, and tailored intervention. This paper presents a simplified map of evidence-informed strategies designed to support immunisation programme managers and health care workers in improving vaccine acceptance at the population and individual patient levels.
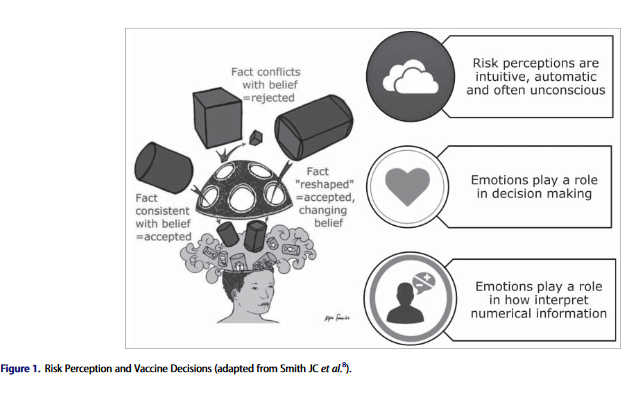
The opening section of the paper outlines some of the challenges. For example, anti-vaccine crusaders can widely share their beliefs on the internet, and social media such Twitter are replete with anti-vaccine sentiments and links to anti-vaccine websites and blogs. As depicted in the image above, vaccine information campaigns developed to counter these influences that are focused on facts have had only limited impact on hesitancy, as risk perception and vaccine decision making are often made at the unconscious level and more influenced by emotions and beliefs.
Some efforts to increase vaccine acceptance have perhaps fallen flat due to their failure to account for factors such as these:
- Vaccine acceptance does not mean hesitancy is not present. Thus, "activation", or setting the social environment for nudge towards acceptance, is important.
- Tailored, multipronged strategies are more effective than single interventions across a broad population.
- Strategies to increase vaccine acceptance need to incorporate respect - indeed, empathy - for different perspectives on immunisation. "[P]olarizing views by arguing aggressively about factual misconceptions is decidedly unhelpful in addressing hesitancy to improve vaccine acceptance."
Other points for immunisation programme managers and healthcare professionals to keep in mind:
- Evaluation is crucial to ensure that interventions designed to address hesitancy work as intended and that adjustment and change can then be made to optimise the outcomes.
- It is important to not neglect the vaccine accepting group, who need to have their vaccine decisions valued and reinforced in order to enhance their resiliency in the face of anti-vaccine messages and sentiments. In addition, acceptors can be powerful allies by advocating its importance for their own family and the community, reinforcing or setting the pro-vaccine social norm to nudge for vaccine acceptance.
The paper outlines a total of 12 evidence-based strategies:
At the programme level:
- Detect and address hesitancy in the population/subgroups. The World Health Organization Regional Office of Europe (WHO EURO) developed the Guide to Tailoring Immunization Programs (see Related Summaries, below) to help countries detect subgroups with low immunisation, diagnose the hesitancy factors, and then intervene with a tailored programme that specifically addresses the factors leading to low vaccine acceptance in the subgroup.
- Ensure all health care professionals know and use best immunisation practices. Considering that healthcare workers can themselves be hesitant, immunisation programmes need to work with partners to optimise training of healthcare students and to provide continuing education in vaccinology for healthcare professionals in practice to ensure that patients receive consistent and accurate messages about vaccines, given in a respectful and positive manner.
- Use specific strategies known to increase uptake, such as (i) engaging community leaders, religious, or other influential leaders to promote vaccination in the community, and (ii) improving convenience and access to immunisation.
- Use effective communication that: is proactive (not reactive), has a focus on listening (not unidirectional provision of information), is tailored to fit the intended audience and the problem being addressed, uses new media and stories (not just facts) where appropriate, and includes messages that are targeted and tested.
- Educate children on the importance immunisation for health.
- Work collaboratively with healthcare professional societies, academia, global agencies, and others who support immunisation; this can add positive voices to the immunisation public conversation.
At the individual/patient level:
- Ensure healthcare professionals know their impact on vaccine decision making. One study found that vaccine information and assurances from a healthcare professional were the main reason why parents who planned to delay or refuse a vaccine for their child changed their minds.
- Do not dismiss a family or patient from the practice because they are hesitant or vaccine refusers. There are legal implications and ethical issues at the individual and population levels as well as potential negative population health implications of dismissal from care.
- Use effective parent/patient discussion-communication techniques. It has been shown that a presumptive approach (e.g., "Sarah is due for immunisation today") is more effective than a participatory approach (e.g., "What do you want to do about vaccination?"). Motivational interviewing is one strategy to be considered when a parent or patient is indeed hesitant.
- Use clear language, and be aware of effects of framing. Pictorial examples of numbers and size may help explain risk better than percentages and fractions. With respect to vaccine safety, it is more effective to say this vaccine is more than 99.9% safe than that it has less than 0.1% serious side effects. However, when discussing vaccine benefits and risks and the risks of vaccine-preventable diseases, telling the truth is an imperative if trust is to be maintained. In summing up the discussion with the parent/patient, the healthcare provider can help the parent/patient with comprehension and recall by emphasising the bottom-line take home message (e.g. the reason this is important is...).
- Reinforce the important of role community protection - but not at the expense of noting the value to the vaccine for the individual patient. There are a number of videos, both humorous and serious, that can help parents understand more fully if interested.
- Address pain associated with immunisation. Evidence-based ways to mitigate pain offer options for all age groups, and some interventions (e.g., as distraction and proper positioning) add no additional cost or time to the procedure.
In conclusion: "Immunization program managers and health care workers need to become adept at recognizing and tackling hesitancy in all of its incarnations if high levels of vaccine acceptance are to be achieved. At the same time,...[b]uilding vaccine acceptance resiliency needs to be part of addressing hesitancy."
Human Vaccines and Immunotherpeutics. 2018; 14(1): 218-224. doi: 10.1080/21645515.2017.1394533. Image credit: Figure 1 from the paper, adapted from Smith JC et al.
- Log in to post comments












































