A People's Vaccine for Refugees: Ensuring Access to COVID-19 Vaccines for Refugees and Other Displaced People
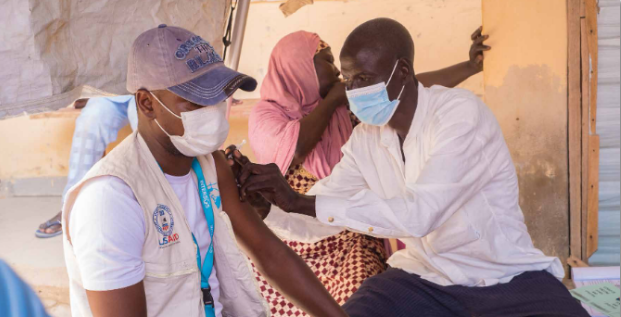
Oxfam International
"[I]nclusion on paper in vaccine roll-outs is not translating into equitable vaccine access for displaced populations in practice..."
This Oxfam briefing note addresses some of the challenges faced by displaced people - including refugees, asylum seekers, internally displaced persons (IDPs), stateless people, and others in displacement contexts - in accessing COVID-19 vaccinations. It identifies a range barriers, explores the issue of lack of information and vaccine hesitancy, and provides recommendations to ensure vaccine access for all displaced people.
Examples of barriers include:
- Administrative - The requirement to show a valid identity document, residence permit, or insurance card prevents many displaced people from registering for or receiving vaccines. Lack of computer or internet access, illiteracy, and language barriers may also prevent these populations from registering for a vaccination appointment, especially when doing so is only possible via online systems.
- Logistical - For example, around 94% of refugees in Uganda live in settlements outside of urban centres. Ugandan government policy aims to have a health centre in every parish, but the health centres closest to most refugee communities are not providing vaccines - often because they lack the refrigeration required to store them. As a result, refugees in remote settlements usually need to travel long distances to access vaccines; the limited transport options present even greater challenges for some of those most vulnerable to COVID-19, such as the elderly and people with certain illnesses or disabilities, in getting to distant vaccine centres.
- Informational and demand-related: A lack of government outreach to displaced communities has left many people without knowledge of where or how to access COVID-19 vaccines or whether they are even eligible to receive one. For instance, in Australia, information about how to receive the vaccine, particularly for vulnerable groups, has been communicated through government advertising and general practitioners (GPs), but many refugees may not engage with such advertising and/or may lack an established relationship with a GP. Inability to discuss concerns with medical professionals and a lack of trust in the authorities have at times hampered attempts to address misinformation around COVID-19 vaccines. Vaccine hesitancy in displaced populations is caused not only by misinformation but also by legitimate concerns about negative interactions with authorities or lack of access to health services (leading some to view vaccination with suspicion).
- Gender-specific: There may be a number of factors contributing to reduced vaccine uptake for women in displaced populations, including:
- There are often gender gaps in access to information and to the technology needed to access information about vaccines or registration.
- Male heads of household may control decision making as to whether the whole family receives the vaccine or whether female family members can travel for this purpose.
- Vaccination centres, especially those far away from women's homes or that are open at inconvenient hours, may not be accessible to women who work mainly in the home or who face mobility restrictions or safety risks.
- Misinformation around vaccine dangers, such as myths that COVID-19 vaccines cause infertility in women or loss of pregnancy, is often gender-specific, creating particular fears for women.
Engaging communities and refugees in vaccine roll-out is identified as the key to success - for example, New Women Connectors, an initiative led by migrant and refugee women, launched its Vaccines4All All4Vaccines campaign in May 2021. The initiative reinforces the right of refugees to know about why and how to get vaccinated and helps institutions understand how to reach out to refugee communities with vaccination campaigns. To do this, it engages in a range of community activities, including holding focus group discussions, mapping vaccine accessibility, translating information about vaccines into refugees' languages, and organising vaccine information both online and offline.
The brief offers recommendations, including those specific to governments of refugee-hosting nations and the international community. But all actors are urged to:
- Actively seek to engage displaced people, and incorporate their voices into vaccine planning: Community leaders, refugee-led and women-led organisations, and local non-governmental organisations (NGOs) need to be meaningfully involved in vaccine roll-out efforts at the local, regional, national, and international levels. For one thing, displaced people are also vital partners in assessing the needs of their communities (including accurately identifying barriers to vaccine access) and undertaking outreach in local languages and culturally appropriate ways.
- Make efforts to deliver targeted vaccine campaigns at the community level: To build trust in vaccine campaigns, governments should work collaboratively with civil society organisations (CSOs) and displaced communities to conduct information and outreach campaigns and vaccination programmes.
- Include women's voices in vaccine planning, and recognise the important role women in displaced communities play in ensuring successful vaccine campaigns: Women need to be included in COVID-19 taskforces, bodies, and committees to effectively identify and address barriers to access for women and girls in all their diversity. It is also important to recognise and support the role and safety of semi-formal and informal health workers - an estimated 70% of whom are women - as part of COVID-19 vaccine roll-out strategies.
Oxfam Policy & Practice website, December 2 2021; and email from Charlotte Greener to The Communication Initiative on January 24 2022. Image credit: Oxfam
- Log in to post comments












































