Vaccine Hesitancy: Where We Are and Where We Are Going
University of Colorado School of Medicine (McClure); University of Colorado Denver (Cataldi); and University of Colorado Denver/Anschutz Medical Campus, Children's Hospital Colorado/University of Colorado School of Medicine, and Adult and Child Consortium for Health Outcomes Research and Delivery Science (O'Leary)
"Use of behavior change principles and communication strategies such as motivational interviewing represent promising approaches to address vaccine hesitancy at the individual level."
This review of literature from 1999 to 2017 focuses on vaccine hesitancy and refusal in the childhood vaccine schedule in the United States (US), although many of the concepts discussed are applicable in other countries and for adult vaccination. Vaccine hesitancy is understood to be a spectrum of parental beliefs and concerns caused by factors including the fact that, as rates of vaccine preventable diseases dwindle, caregivers may grow to fear the vaccine more than the disease it prevents. In addition, highly publicised antivaccine arguments have caused public backlash against vaccines. The internet is filled with information about the dangers of vaccines, which can leave parents with mixed messages and uncertain of which sources to trust. The medical community's inability to influence vaccine decisions simply by correcting misinformation is well documented.
The review looks at strategies to address vaccine hesitancy that have been examined in the literature. Despite much work across disciplines showing that simply providing information often does not lead to people changing their views and may even create a dynamic in which a patient or parent is actually less receptive to information a provider may impart, it has been found that medical providers are a trusted source of information about vaccines. Building a trusting relationship with parents and patients can promote vaccine acceptance and also influence other important aspects of care. There is tension in how current research guides paediatricians in their vaccine discussions. On one hand, it seems that the presumptive approach, which assume parental consent to vaccines, improves vaccine uptake. On the other hand, research has also documented that parents often expect a more engaged, open-ended approach to vaccine discussions, and some evidence suggests that a presumptive approach may lead to decreased parent visit satisfaction.
Motivational interviewing is described here as "the process of engaging in an open-ended discussion with an individual to assess an individual's readiness to change with the goal of drawing upon the person's own desire and motivation to change, rather than the provider's motivation." On this approach, if a provider is interacting with a vaccine-hesitant parent who has just described his or her concerns regarding vaccination, instead of attempting to respond with persuasive arguments or lecturing with facts, the provider would "continue to create a welcoming, nonthreatening environment by reflecting back the parent's concerns. As the parent demonstrates willingness to further engage in the conversation, the provider can strategically pivot the conversation from the parent's concerns (which the provider has already assured the parent that he or she has heard and understands) to disease process at hand, because there is some evidence that focusing on the disease rather than the barrier is more likely to improve intention to vaccinate."
The review looks at immunisation laws and school exemptions, as well as dismissal from a physician's practice of families who refuse vaccination, before exploring the topic of nudges for behaviour change. The presumptive approach to communication about vaccines can be seen as a nudge because it alters how the choice is presented but does not eliminate the option to decline vaccines. Some have argued that nudges are a gentle subversion of patient autonomy, whereas others emphasise that nudges are acceptable as long as they adhere to the principle of promoting the best interest of the patient.
One section of the review looks at behaviour change theories, such as the Theory of Planned Behavior, and their role in addressing vaccine hesitancy. "The psychological concept of values describes priorities and beliefs that motivate personal attitudes and behaviors but are more constant throughout situations and time....Aligning with personal values may improve communication of scientific ideas, including information about vaccines....Preliminary work to apply personal values to childhood vaccination has succeeded in establishing a framework of immunization values that are associated with vaccine hesitancy and with delayed vaccination behavior." Similarly, social norms have been found to be successful in promoting vaccination. The presumptive approach to vaccine conversations in a medical office relies upon the assumption that vaccination is the default choice (i.e., the social norm). In Washington, US, a programme called Immunity Community trains parents who support vaccination to be communicators and advocates in their local communities. In Colorado, Parents for Vaccinated Communities works to engage parents in advocacy to support vaccination. "These community engagement projects show promise in harnessing the energy of parents who vaccinate to counter vaccine hesitancy and refusal and to promote vaccination as a social norm."
Tips for communicating with parents about vaccines are offered, including:
- Keep it conversational - avoid launching into a lecture full of facts about vaccines.
- Beware when debunking myths - too much time talking about a vaccine myth can actually strengthen the myth in the listener's mind.
- Rather than refuting incorrect elements of existing beliefs, try to provide new information to replace those elements.
- Use personal anecdotes and stories (e.g., a physician talking about the decision to vaccinate his or her own children), which are powerful communication tools.
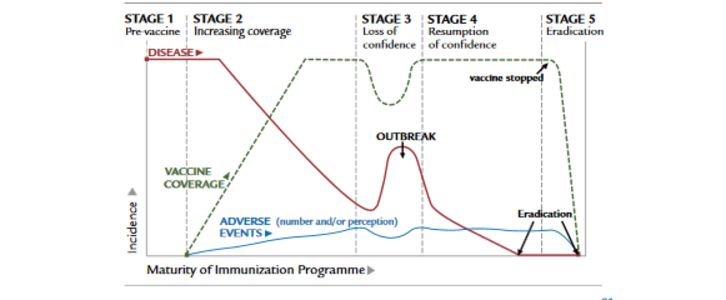
Clinical Therapeutics, Volume 39, Issue 8, Pages 1550-1562. DOI: https://doi.org/10.1016/j.clinthera.2017.07.003. Image credit: This image was reprinted with permission for the above-summarised article by the authors of that article from Chen, R.T., Rastogi, S.C., Mullen, J.R. et al, The Vaccine Adverse Event Reporting System (VAERS). Vaccine. 1994;12:542–550.
- Log in to post comments












































