Project Muso Community Based Malaria Program
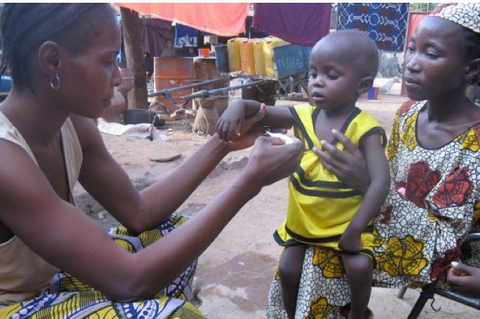
Operating since 2007, Project Muso's Community Based Malaria Program is a community-led system for malaria prevention and treatment in Yirimadjo, Mali working to reduce malaria deaths by strengthening the primary health care system as a whole, providing education about malaria prevention, and providing universal bednet coverage to all community members. The project is organised around three principle strategies: assisting Community Health Workers (CHWs) to provide home-based diagnosis and treatment; operating a Solidarity Fund to remove financial barriers; and strengthening clinical infrastructure. Community Health Workers are local mothers who are trained, supervised, and supported to extend primary health care into the homes of community members.
Community Health Workers are an important part of the Project Muso strategy, significantly expanding the local healthcare force. CHWs receive training in malaria prevention, diagnosis, and treatment. As neighbours, they are trusted and respected women who spend at least two hours a day conducting door-to-door outreach in their communities, finding, diagnosing, and treating cases of simple paediatric malaria, bringing patients with severe malaria and other illness into the CSCOM (community health centre), and educating families on malaria prevention and basic health and hygiene practices. They have been trained to use Malaria Rapid Diagnostic Testing to identify plasmodium falciparum malaria in children younger than five and to administer home treatment with ACT.
According to Project Muso, Mobile CHWs make home-based care much more effective because they have the capacity to communicate effectively with patients and build trusting relationships that promote lasting behaviour change. CHWs follow a rigorous protocol of fever evaluation, rapid antigen malaria diagnostic testing using a finger-prick assay, and on-site treatment with ACTs. Their responsibilities include the following:
- conducting regular home visits with families to discuss malaria prevention and treatment;
- determining which pregnant women and children younger than five are not sleeping each night under a LLIN, and providing information, training, and resources necessary to achieve nightly bed net use for these populations;
- identifying simple malaria cases among children younger than five via diagnosis using rapid antigen assay tests;
- administering ACT within 24 hours of symptom onset for children younger than five with positive rapid tests;
- following up with each patient within 24, 48, and 72 hours of treatment to track progress and determine future steps;
- identifying pregnancies early, referring pregnant women to the health center for prenatal consultations, providing counselling and follow-up to promote healthy pregnancy, and ensuring intermittent preventative malaria prophylaxis adherence; and
- tracking births and deaths in the community.
Project Muso also builds on their relationships with local leaders by connecting local religious leaders and their faith communities with the Community Health Worker in their area. By connecting Community Health Workers to help those in need in their communities, religious leaders are an important connection for active referrals and rapid case findings to the CHWs.
Since 2007, Project Muso has been delivering bednets at eight distribution points in Yirimadjo in collaboration with local and community partners. All net distributions have occured in close collaboration with the Yirimadjo Community Health Center and the Community Action Committee. Along with the CHWs, a network of Community Health Promoters have been trained to assist with efficiently distributing nets and teaching the community skills in the prevention and treatment of malaria via theater pieces, one-on-one trainings, and training with community members in their homes.
Malaria
According to Project Muso, although it is a preventable and treatable disease, malaria in Yirimadjo is a primary cause of suffering and death, accounting for 63% of healthcare demand. Although Mali's government has invested in malaria medicine and bednets for children and pregnant women, growing evidence indicates that this is not enough to achieve malaria control. Effective healthcare delivery systems must be tested and scaled up to ensure that community members access and use these powerful interventions. People don't seek care because they have malaria, they seek care because they feel sick. When high quality primary health care is available and accessible, communities develop increased trust in the health system, which results in increased use of primary care as well as earlier treatment for specific priority diseases such as malaria.
Project Muso, the Against Malaria Foundation, the Conservation, Food & Health Foundation, Rotary International Future Visions
Project Muso website on June 11 2012.
- Log in to post comments












































