HPV-Related Cancer Prevention and Control Programs at Community-Based HIV/AIDS Service Organizations: Implications for Future Engagement
Texas A&M University (Wigfall, Sebastian, Ory); National Institutes of Health (Bynum); University of South Carolina (Brandt)
"[T]he potential for ASO staff to help their clients overcome barriers and enable them to make informed (or at a minimum shared) decisions about cancer screening with their health care providers becomes increasingly important..."
People living with HIV/AIDS (PLWH) and men who have sex with men (MSM) are disproportionately affected by genital warts and cancers caused by human papillomavirus (HPV). Community-based HIV/AIDS service organisations (ASOs) provide PLWH, MSM, and other vulnerable populations with resources such as health education, patient navigation, and social support. This study assessed community-based ASOs' staff awareness, knowledge, attitudes, and beliefs about HPV and effective cancer prevention tools, namely HPV vaccination, Pap, and HPV tests. The researchers also explored the potential engagement of ASO staff in future efforts to reduce the disproportionate burden of genital warts and HPV-related cancers among HIV-positive women and MSM.
In May-June 2016, 30 staff were recruited from 3 ASOs located in the South United States (US) Census region - a geographical area disproportionately affected by HIV/AIDS. Participants completed a 30-minute, self-administered, 118-item paper-and-pencil survey about HPV and cancer.
All participating ASO staff reported hearing of HPV, and 77% had heard of the HPV vaccine (n = 23). While all knew HPV can cause cervical cancer, only 67% knew HPV can cause anal cancer. Most (61%) thought the HPV vaccine could prevent cervical cancer. Fewer (39-48%) thought the HPV vaccine could prevent anal, oral, penile, vaginal, and vulvar cancers. Although 70% of ASO staff knew that the HPV vaccine was recommended for PLWH aged 9-26 years, far fewer thought the HPV vaccine was safe (52%) and effective (43%).
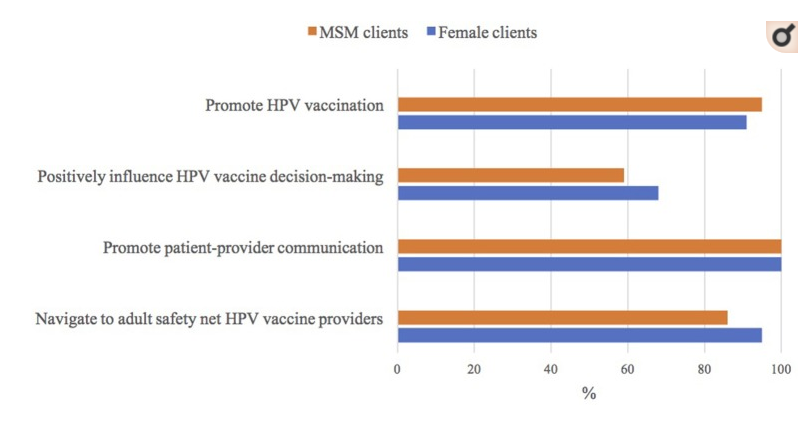
All ASO staff were willing to encourage their female and MSM clients to talk to their healthcare providers about the HPV vaccine. A larger percentage of ASO staff who worked with MSM clients (95%) were willing to encourage these males to get the HPV vaccine, compared to ASO staff who worked with female clients (91%; p = 0.47). In contrast, a smaller proportion of ASO staff who worked with MSM clients thought their opinion could influence these males' HPV vaccine decision-making (59%) than ASO staff who worked with female clients (68%; p = 0.37). Similarly, a smaller proportion of ASO staff who worked with MSM clients were willing to help navigate these males to adult safety net HPV vaccine providers (86%) where they could get the HPV vaccine for free or at a reduced cost than those who worked with female clients (95%; p = 0.06).
The researchers indicate that further investigation is needed to better understand how to integrate HPV-related cancer prevention education into existing services provided by ASO staff, which include HIV/sexually transmitted infection (STI) testing and risk-reduction counseling for both PLWH and high-risk HIV-negative persons. Because many ASO staff also help their clients link to healthcare providers where they can receive needed healthcare services such as HIV care and pre-exposure prophylaxis (PrEP) clinics, the integration of patient navigation to adult HPV vaccination safety net providers and other cancer care providers where they can receive screening, diagnostic, and treatment services also warrants further study.
In conclusion: "Engaging ASO staff in cancer prevention efforts may increase HPV vaccination rates and early detection of HPV-related cancers among HIV-positive women and MSM."
Frontiers in Oncology. 8:422. doi: 10.3389/fonc.2018.00422.
- Log in to post comments












































